Why do I need to keep a dressing on my leg?
The dressing will protect your wound from the environment, reducing the risk of infection. It will also help to manage any symptoms that might be causing you problems such as wound fluid or odour. Finally, it will create a moist environment which promotes quicker healing.
Won’t it be better to let the air get to the wound?
Moist wound healing has been shown to be the best environment for wound healing in the majority of people. Maintaining an environment that is not too wet or dry increases the speed of healing. Your healthcare professional will help you to select a dressing to achieve the perfect balance for your wound.
Why is it important that I keep wearing compression hosiery once my leg ulcer heals?
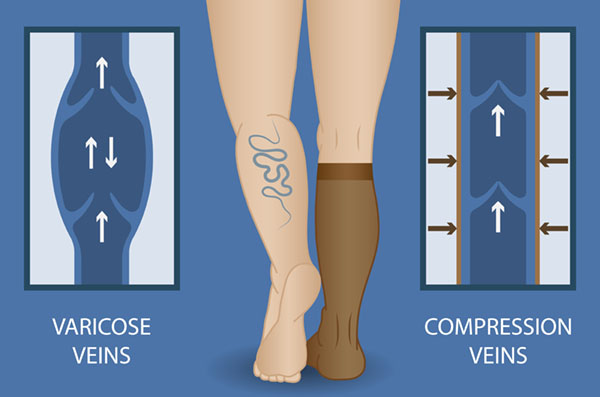
Compression hosiery addresses the underlying cause of venous ulceration, by helping to improve the return of blood from the limb to the heart. Once your ulcer is healed, the underlying cause is still there. For this reason, you should continue to wear your garment. Evidence shows that people who wear compression following healing have a lower rate of recurrence than those who don’t.
I find the compression bandages restrictive and miss daily showers, why do I have to wear them continuously?
Bandaging can be bulky, hot and uncomfortable as well as inconvenient. Remember if you need to wear bandaging, it is not forever, just until your limb size has reduced and/or your wound has reduced in size enough to not need bulky dressings.
I find my legs itchy and dry around the wound site, what can I do to relieve the symptoms?
Good skin care in the form of cleansing and moisturising can help to alleviate some of these symptoms. Be sure to use bland emollients and make sure they do not affect your compression garment by applying in advance of wearing your garment.